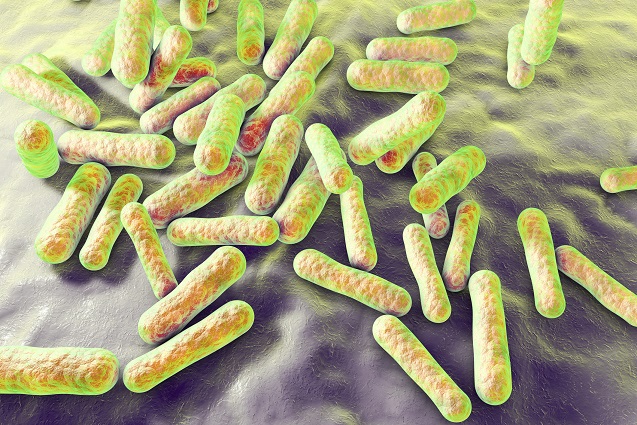
 The role of p.acnes bacteria in acne is well known. It inhabits your sebaceous glands and when overgrown, stimulates an immune system response which inflames and swells your pores. But up until about twenty years ago there remained some mystery, since p.acnes is also a perfectly normal member of human skin flora.
The role of p.acnes bacteria in acne is well known. It inhabits your sebaceous glands and when overgrown, stimulates an immune system response which inflames and swells your pores. But up until about twenty years ago there remained some mystery, since p.acnes is also a perfectly normal member of human skin flora.
You need p.acnes to prevent clogged pores and to kill infectious viruses. Even the most perfect skin pore in the world contains a bacterial composition of 87% p.acnes. What’s strangest is that occasionally, studies show that clear-skinned people and acne-ridden teenagers have the exact same levels of p.acnes bacteria, despite their wildly different skin quality.
What’s the explanation? Like all infectious bacteria, such as the mostly benign E.coli where only a few subspecies actually kill people, Propionibacterium acnes has countless different strains and some are much more involved with acne than others.
The truth about p.acnes bacteria
 P.acnes bacteria is not one uniform microorganism, nowhere close to it. The strains share countless broad characteristics, such as feeding off sebum for their energy, but there’s 4 main subgroups of p.acnes and over 11,000 different types have been detected in human skin.
P.acnes bacteria is not one uniform microorganism, nowhere close to it. The strains share countless broad characteristics, such as feeding off sebum for their energy, but there’s 4 main subgroups of p.acnes and over 11,000 different types have been detected in human skin.
While researching solutions for acne, including on this website, you’ll see advice that honey kills p.acnes, blue light devices kill p.acnes, and so on. The reality of p.acnes is far more complex than those statements suggest. Some types of p.acnes can trigger acne, while others have no effect at all even if their populations are out of control.
The most recent illustration was an overhyped but excellent study released back in 2013. Multiple strains of p.acnes bacteria were analysed, including 66 previously undetected strains. This alone shows how multiple new strains are constantly being discovered. The 10 most common ribotypes (strains) of p.acnes were analysed in detail. These bacteria samples were obtained from 52 people with clear skin and 49 people with acne ranging from moderate to severe.
Read Annihilate Your Acne – get the diet that could transform your skin!
Strains 1, 2, and 3 were all found in equal amounts in healthy and acne-prone skin. Meanwhile, strains 4, 5, 7, 8, 9, and 10 were much more concentrated in acne-ridden skin. Strain 6 was most prevalent in healthy skin.
The most closely connected strains to acne were 4 and 5, as 20% of patients with severe acne had colonies of them, compared to almost zero for people with clear skin.
On one hand, there was strain 4, where 84% of total samples came from acne patients compared to only 16% from clear skinned humans. On the other, there was the beneficial strain 6, where a mere 1% was isolated from acne patients compared to 99% from healthy skin samples.
Then despite being deemed less to blame for acne than strain four, 100% of strain 8 and 10 samples were discovered in acne patients, while 0% were detected in healthy people. Also observed were 5 different microbiomes, broad compositions of facial bacteria. Microbiomes 4 and 5 were mostly closely associated with acne; these two were the richest in strains 4 and 5 as well.
A lot of people were shocked by this study, but the research has actually been simmering away since the early 2000s, when p.acnes bacteria was separated into 4 broad categories: 1a, 1b, 2 and 3.
Acne-prone skin is far more likely to contain members of subgroups 1a, and almost never subgroup 3. A gang of scientists once collected 106 strains of p.acnes from Danish skin. 25 from skin samples with severe acne, 42 from mild acne, and 39 from healthy skin.
Among the severe acne isolates, 22 belonged to p.acnes division 1a. Three were from the combined divisions of 1b and 2, while none were isolated from division 3.
There’s even variation within this sinister 1a sect. One group called complex 18 from the 1a subgroup, a complex which itself contained a huge 46 different strains, had 30% of its detected occurrences come from extreme acne. For complexes 27 and 28, also from 1a, the figure was 7.1%.
The conclusion is clear: some strains of p.acnes are much more troublesome than others.
But why?
The 2013 study found that all 10 main ribotypes were 99% identical to ribotype 1 genetically. But that means little; remember that an Alaskan brown bear is almost 99% genetically identical to Polar bear. Genetic differences are confirmed; a type 1a strain called sk137 was observed to be far more prevalent in acne patients compared to type 1b strain KPA171202. Sk137 had 64 unique genes, while KPA171202 had 124 unique genes.
What we care even more about is the mechanism though, and summarised simply, the sinister strains of p.acnes such as subspecies 1a stimulate a far stronger pro-inflammatory response from the immune system. They therefore also stimulate more acne, since chronic inflammation is the fuel for the acne fire in the initial stages, the kick-starter of the whole pimple process.
First there’s human beta-defensin (hBD). This peptide is secreted by skin cells to kill many microorganisms, including p.acnes bacteria, in spite of the fact that hBD is actually incapable of killing p.acnes. HBD can be a huge factor in inflammation and thus acne, partly because after being dispatched it attracts numerous other inflammatory chemicals like a magnet, such as neutrophils. This study observed that type 1a and 1b p.acnes bacteria increased hBD secretion fivefold after just 3 hours, but type 2 caused no increase whatsoever.
Next – the 6 best vitamins and minerals for naturally clear skin
Another pro-inflammatory chemical is interleukin 8, a chemical which is far too active in people with acne. This time all four p.acnes subgroups stimulated interleukin 8, but there was variation even among the type 1a strains, from a 5.5 fold to a 3 fold increase.
We also have the pro-inflammatory chemical interleukin-1a. None of the four strains increased this agent of acne significantly, but a group 1a strain (strain 2005) increased it two fold compared to a miniscule increase in the 1b strain (p.acnes strain 6609).
Once more, p.acnes group 1a is the most responsible for acne, but there’s variation even within it. Our story continues in a separate study on tumour necrosis factor alpha (TNF-a), where 1a and 1b strains increased it significantly while group 2’s efforts were much more feeble.
All four are bread and butter chemicals involved with acne, in the beginning stages of a pimple’s life, so this is pretty strong evidence already.
The secrets of p.acnes
Then there’s the theories about WHY some trigger so much more inflammation than others: about various proteins, enzymes, and metabolites that different strains naturally produce.
NEURAMINIDASE – one is neuraminidase, an enzyme secreted by p.acnes. Neuraminidases have a pretty obscure role, but what’s more important is they are what’s called an antigen.
That’s a substance which the immune system uses to identify a target; a good example is influenza molecules, which have neuraminidases in their structure that our immune systems have adapted to recognise and target. A good metaphor would be a formerly peace-loving great white shark scenting blood (AKA the antigen) and suddenly entering Jaws-mode.
What does this mean for acne? P.acnes types 1a and 1b are proven to secrete more neuraminidase. This study even found that 90.0% of p.acnes strains from acne-prone skin secreted neuraminidase, compared to 72.7% in healthy skin. The more neuraminidase is being secreted onto your skin’s surface, the more stimulation there is for your immune system to inflame it and cause acne, with hBD, IL-8 and all the rest.
DERMATAN-SULPHATE-BINDING-PROTEIN – DS-BP is a molecule which binds to dermatan sulphate and prevents it from working. Dermatan sulphate is a glycosaminoglycan, a substance involved with wound repair and skin structure.
7 natural topical treatments which could transform your skin
P.acnes secretes DS-binding protein, for mysterious reasons, but possibly because dermatan sulphate contains a nutrient which p.acnes wants to extract and consume. More importantly, DS-BP is strong antigen just like neuraminidase. It makes sense, since the immune system obviously won’t like a compound which makes your skin crumble to dust. Type 1a and 1b p.acnes secrete DS-BPs, but types 2 and 3 do not.
LIPASES – the most ubiquitous of these substances is lipase. Lipases are enzymes which break down fatty acids, which you yourself have in your stomach to digest fats in food. P.acnes bacteria also secretes lipases in order to digest their main energy source, sebum…
…but type 1a strains such as strain complex 18 significantly overproduce them, while type 2 strains produce much less. They overproduce a specific lipase called glycerol-ester hydrolase A (gehA), used to break down sebum triglycerides. They thus also overproduce inflammatory metabolites of sebum breakdown like glycerol and free fatty acids.
LIPOGLYCANS – lipoglycans, also known lipopolysaccharides, are proteins which are one of the main antigens used by the immune system to identify bacteria. Lipoglycans have been proven again and again to induce an inflammatory immune system response; they’re much better researched than the two antigens above. They are the kings of the antigens, produced by countless bacteria.
The most important thing to know – type 1a and 1b p.acnes pump out significantly more lipoglycans than type 2.
We have some solid explanations for the extra inflammation from certain p.acnes strains, which itself was a solid explanation for the increased acne.
It doesn’t end here as these are only the clear factors. Type 1a p.acnes lacks 10 genes associated with carbohydrate metabolism; maybe that’s why it produces extra lipase, to obtain more energy from fat instead. Type 2 p.acnes lacks the sugar galactose in its outer cell wall. P.acnes strains also secrete proteins with wildly varying compositions of amino acids.
Are these differences consequential? Not necessarily, because propionibacterium acnes wasn’t created by nature solely to give us acne. It’s just another microorganism trying to survive and these differences may be completely unrelated. Make no mistake though, that there’s more to this bacteria than what meets the eye.
The benefits of p.acnes
 Just as some strains of p.acnes are worse than others, many have protective powers. In fact p.acnes is very healthy for human skin on the whole, which is why all skin contains it. It’s excessive levels and as we now know, the dodgy strains which wreak acne havoc.
Just as some strains of p.acnes are worse than others, many have protective powers. In fact p.acnes is very healthy for human skin on the whole, which is why all skin contains it. It’s excessive levels and as we now know, the dodgy strains which wreak acne havoc.
The consumption of sebum is a nice gift as this normally keeps your skin pores open, even if its reasons are selfish, to obtain energy. Before the dawn of antibiotics, the inevitable p.acnes growth that resulted from this feast would be kept in check by blue light.
P. acnes also keeps your skin’s immune system energised, on its toes for more deadly threats, through constant stimulation. More interesting is that p.acnes manufactures its own bacteriocins, or bacteriocin-like compounds, such as acnecin, propionicin PLG-1, bacteriocin RTT108 and jenseniin G.
Zinc – the number one mineral for clear skin (reduces acne by 49.8%)
These are active against other skin flora microorganisms without harming our own skin. Targets include various yeasts, moulds, and infectious bacteria. The exact roles of these bacteriocins remains shrouded in darkness, but acnecin is known to act against other members of the p.acnes family (perhaps it protects against the unhealthy strains), while bacteriocin RTT108 impacts a far wider set of bacteria, both gram positive and negative.
So while p.acnes might give you acne when in world domination mode, healthy amounts protect you against much worse things.
More interesting facts
Another interesting characteristic of p.acnes bacteria is the lack of diversity around the world. Somehow, p.acnes has spread so far and wide that the skin flora of a Chinaman in Beijing is hardly any different to a Scandinavian in a mountain hut. Subgroups such as 1a and 3 occur in fairly equal quantities around the world. Gut flora, meanwhile, is known to be more regional.
Now surely there’s a clear explanation here: p.acnes lives on the skin’s surface, people touch and rub their face constantly, and it must be easy for p.acnes to spread from human to human in airports, and thus all over the world. It has previously been observed that p.acnes cross infects visitors to dermatology clinics, both directly and indirectly. Presumably the effect here would be NEGATIVE because all the visitors will have acne, so that’s yet another reason to rely on natural methods.
Another interesting phenomenon relates to antibiotic resistance, the ever growing epidemic. Many strains of p.acnes bacteria now contain a gene which confers increased resistance to the widely prescribed antibiotic tetracycline. In the 2013 study, this was heavily found in ribotypes 4 and 5, the two worst strains for acne.
Additionally, patients who had never even taken antibiotics had these antibiotic resistant strains. It is thus clear that the pandemic of antibiotic resistance is spreading far and wide. However, it remains strain specific, with 4, 5, and 10 being the most resistant, so by a stroke of luck, some people might contain the strains which are holding out.
What does this mean for acne?
Firstly, let’s cast aside the fact that p.acnes bacteria is only one piece of the clear skin puzzle, since we’ve discussed that in detail elsewhere.
Focussing strictly on p.acnes, no studies to date have taken advantage of this interesting phenomenon. RIGHT NOW there are no prospects at all, but in the future, it’s very possible that we can target and wipe out the deadliest strains of p.acnes, and thus target acne like a laser rather than a shotgun.
Such a treatment is possible; with numerous physical differences between the strains, like the absence of carbohydrates in the cell walls, or differing proteins, scientists with all their ingenuity will surely come up with a way to take advantage. The only problem is this: when this mysterious treatment does come around, it will almost certainly be synthetic to begin with, a drug created in a lab…
…and like benzoyl peroxide or Accutane there will surely be many side effects which emerge over time. So the best prospects are in the natural world of acne treatments. But there’s a problem there too: what plant or herb will happen to have the exact profile of nutrients optimal for killing one strain of p.acnes over the other? Broad antibacterial powers like those in raw honey or blue light devices are one thing, this is far more specific.
There are some interesting studies though: the lipases secreted by p.acnes were found to be strongly inhibited by the flavonoid antioxidants catechin and kaempferol (study), while plant saponins glycyrrhicic acid (found in licorice root) and digitonin had little effect.
So for us, the best treatment could be a cream compiled of other compounds like this, compounds which inhibit neuraminidase, lipases, DS-BP, and other differentiating factors in p.acnes which will surely be discovered soon. It won’t be natural but the ingredients will be; it will be free from harsh manmade chemicals.
What happens next though? Will inhibiting specific p.acnes strains even achieve much, compared to inhibiting every single strain?
Some acne patients would benefit much more than others. The most pathogenic p.acnes strains are concentrated in acne patients, but it’s still possible that one person with moderate acne has a much healthier skin flora compared to another. Our first patient’s acne might be more related to chronic inflammation, his immune system overreacting to the comparatively healthy strains, whereas our second person might have a more restrained immune system, but a far more sinister microbiome.
So even if their acne levels are identical, person A will benefit somewhat from killing p.acnes with our futuristic strain cream, but nowhere near as much person B. Person A would be wise to focus on anti-inflammatory treatments like aloe vera instead.
That theory applies to overall p.acnes levels, but with the strain diversity we’ve just added another layer of mystery. So heed this: with such complexity and unknown factors around, it reiterates that experience is a very important thing in acne. Antibacterial treatments just got more unpredictable than ever, and if you’re using raw honey you need to watch your skin like a hawk.
Conclusion
There’s much more to the p.acnes bacteria story than many people realise. It isn’t one uniform strain, determined to ruin everybody’s skin. P.acnes is just as biodiverse as everything else in nature.
Even if we can’t take advantage of the information here yet, it’s always great to accumulate more and more knowledge. One practical usage this does have right now is that it could explain why antibacterial treatments have failed miserably for you. Maybe your pores are utterly clogged and p.acnes is thriving, but the right strains are thriving.
Regardless, you are now more of an expert on acne than ever.
NEXT: discover the root causes of acne and banish your pimples forever
Thanks for reading!